Lupus is a complex and multifaceted autoimmune disorder, where the immune system, which typically protects the body from infections, mistakenly attacks its own tissues. This results in inflammation and damage across various body parts, including the skin, joints, kidneys, heart, lungs, and even the brain. Often referred to as “the disease with a thousand faces,” lupus can appear differently in each person, sometimes making it challenging to diagnose and manage. The condition can range from mild to life-threatening, with symptoms that fluctuate between active disease (flares) and periods of improvement (remission). Understanding lupus is crucial for those affected by it as well as their caregivers, as early diagnosis and effective management can significantly improve quality of life.
Recognizing the Symptoms of Lupus
Lupus manifests with a wide array of symptoms that can vary significantly among individuals. While some might experience a few mild symptoms, others might confront more severe issues. These symptoms can evolve, often unpredictably, and are typically characterized by periods of flares and remissions.
Common Symptoms
- Fatigue: For many, fatigue is the most debilitating symptom. It’s not just about feeling tired; it’s a profound exhaustion that can interfere with daily life, regardless of sufficient rest or sleep.
- Joint Pain and Swelling: Arthralgia and arthritis are prevalent in lupus, often affecting the hands, wrists, and knees. This joint pain is migratory, meaning it can move between different joints over time.
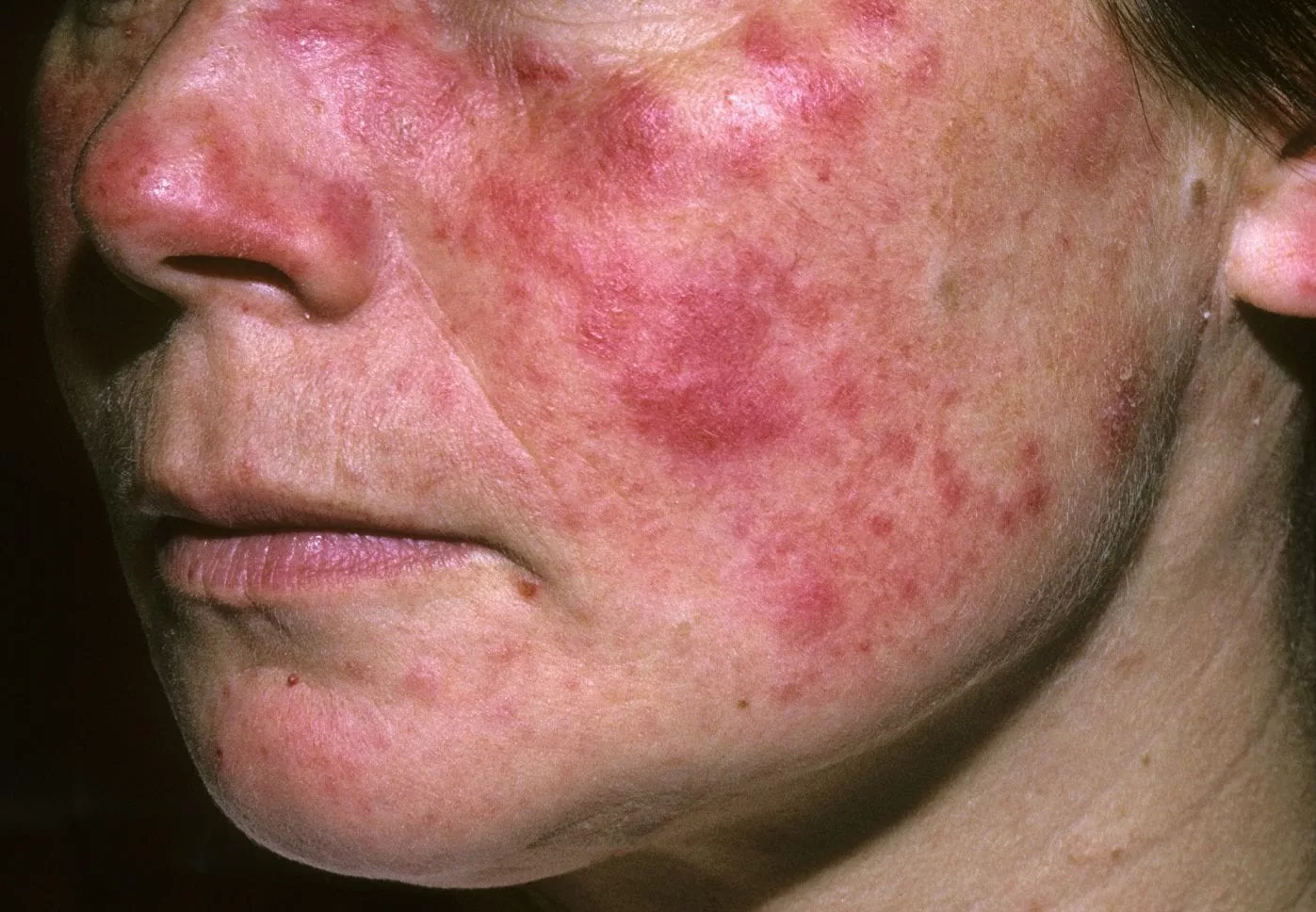
- Skin Rash: One of the hallmark signs of lupus is the butterfly-shaped rash across the cheeks and nose, known as a malar rash. This rash can be aggravated by sun exposure, and other rashes may appear on the face, neck, or arms.
- Fever: Many individuals with lupus experience low-grade fevers that appear without any clear cause.
- Photosensitivity: Sensitivity to sunlight or artificial UV light is common, often leading to skin rashes and triggering flares.
- Hair Loss: Hair thinning or loss during flares is not uncommon, affecting the scalp or body hair, and can sometimes reverse when the condition is controlled.
- Raynaud’s Phenomenon: This condition causes fingers and toes to turn white or blue in response to cold or stress due to restricted blood flow.
- Chest Pain: Inflammation of the lining of the lungs (pleuritis) or heart (pericarditis) can result in chest pain, particularly when taking deep breaths.
Organ-Specific Symptoms
In more severe cases, lupus can target specific organs, leading to complications that may not be immediately apparent but can develop over time.
- Kidney Problems: Lupus nephritis involves kidney inflammation, causing symptoms like swelling in legs and feet, high blood pressure, and foamy urine due to protein leakage. Without treatment, it can progress to kidney failure.
- Neurological Symptoms: Lupus can impact the central nervous system, leading to headaches, memory issues, confusion, seizures, and even strokes.
- Heart and Lung Complications: Inflammation may affect the heart muscle (myocarditis), the heart’s outer lining (pericarditis), or the lungs (pleuritis), increasing the risk of cardiovascular disease.
- Blood Disorders: Lupus can lead to anemia, thrombocytopenia (low platelet count), or leukopenia (low white blood cell count), and increase the risk of blood clots.
Cognitive and Psychological Impact
Beyond physical symptoms, lupus also affects mental and emotional health.
- Cognitive Fog: Many experience “brain fog,” involving difficulty with concentration, memory problems, and trouble processing information.
- Mental Health: The chronic nature of lupus, along with pain and fatigue, can contribute to depression and anxiety, necessitating mental health support.
Managing Symptoms
Effectively managing lupus symptoms involves a combination of medical and lifestyle approaches:
- Symptom Diary: Keeping a detailed log of symptoms can help identify triggers and is useful for healthcare consultations.
- Pacing and Rest: Prioritizing activities and taking regular breaks can help manage fatigue.
- Hydration: Staying well-hydrated supports overall well-being and can alleviate certain symptoms like headaches.
- Mind-Body Practices: Engaging in yoga, tai chi, or meditation can help manage stress and improve mental health.
- Nutritional Support: Ensuring a balanced diet rich in anti-inflammatory foods such as omega-3 fatty acids, found in fish like salmon and walnuts, can help manage symptoms and support immune function. Limiting caffeine and sugar may also reduce fatigue and improve mood stability.
Understanding Types of Lupus
Lupus is an umbrella term for several types of the disease, each with its distinct characteristics. Here’s a look at the different forms:
Systemic Lupus Erythematosus (SLE)
SLE is the most common and severe form of lupus, capable of affecting multiple organs and systems. Its symptoms are diverse, including joint pain, rashes, and severe organ involvement like kidney and neurological issues. Treatment usually involves immune-suppressing medications to manage inflammation and prevent organ damage.
Discoid Lupus Erythematosus (DLE)
Primarily affecting the skin, DLE causes round, disc-shaped rashes that can become scarred. These rashes often appear on the face, scalp, and neck. While DLE typically doesn’t involve internal organs, it can potentially progress to systemic lupus.
Drug-Induced Lupus
This temporary form of lupus arises from specific medications, mimicking SLE symptoms like joint pain and rashes without severe organ damage. Once the medication is stopped, symptoms usually resolve without progressing to systemic lupus.
Neonatal Lupus
A rare condition affecting newborns of mothers with lupus, characterized by skin rashes, liver problems, or low blood cell counts. In some cases, it can lead to congenital heart block. Most symptoms are temporary and resolve over time, although heart issues may persist.
Subacute Cutaneous Lupus Erythematosus (SCLE)
SCLE primarily affects the skin, causing lesions after sun exposure. These lesions typically don’t scar but may be disfiguring and are sometimes associated with mild systemic symptoms. SCLE rarely leads to severe organ involvement.
Advances in Lupus Research
Recent research efforts aim to unravel the genetic and molecular underpinnings of lupus. Scientists are exploring potential biomarkers for earlier diagnosis and personalized treatment. Clinical trials are testing new medications, including biologics, which promise more effective treatments with fewer side effects.
Genetic Insights
Advancements in genomic technologies have allowed researchers to identify specific genetic variations linked to lupus, providing insights into its hereditary nature. Understanding these genetic factors can lead to targeted therapies and improved predictive models for individuals at risk.
Biologics and New Therapies
Biologics represent a promising area of treatment, focusing on precision medicine by targeting specific components of the immune system. These therapies, such as monoclonal antibodies, offer hope for those who do not respond to traditional treatments, potentially reducing the frequency and severity of flares.
Treatment Strategies for Lupus
While there is no cure for lupus, a strategic approach to treatment can help manage symptoms and improve quality of life. Treatment plans are tailored to the individual’s disease severity and organ involvement.
Medications
Medications form the cornerstone of lupus management, targeting inflammation, symptoms, and the immune system:
- NSAIDs: Nonsteroidal anti-inflammatory drugs like ibuprofen help relieve mild joint pain and inflammation.
- Antimalarials: Drugs like hydroxychloroquine manage joint pain, skin rashes, and fatigue, preventing flares and organ damage.
- Corticosteroids: These reduce inflammation quickly but have side effects such as weight gain and osteoporosis with long-term use.
- Immunosuppressants: Medications like azathioprine and methotrexate suppress the immune system, essential for severe cases or organ involvement.
- Biologics: Belimumab targets specific immune cells, offering an option for those unresponsive to standard treatments.
Lifestyle Modifications
In addition to medication, lifestyle changes play a vital role in managing lupus:
- Sun Protection: To prevent flares, protect skin with sunscreen, wear protective clothing, and avoid peak sun hours.
- Regular Exercise: Activities like swimming, walking, or yoga are beneficial for joint mobility and overall health, but avoid overexertion during flares.
- Healthy Diet: A balanced diet rich in anti-inflammatory foods supports immune health. Limit processed foods and saturated fats.
- Stress Management: Techniques like meditation and mindfulness can help reduce stress, which may trigger flares.
- Sleep Hygiene: Ensuring adequate sleep by maintaining a regular sleep schedule, creating a restful environment, and avoiding screen time before bed can improve fatigue and overall health.
Ongoing Care and Monitoring
Due to its complexity, lupus requires regular medical care. Frequent check-ups with a rheumatologist are crucial to monitor disease progression, adjust medications, and detect complications early. Tests like blood work and imaging studies assess organ function and disease activity.
Ensuring Treatment Adherence
- Medication Routine: Consistency in taking medications is key to their effectiveness.
- Pill Organizer: Helps track medication intake and prevents missed doses.
- Stay Informed: Understanding medications and their effects empowers better management and adherence.
- Set Reminders: Utilize smartphone apps or alarm clocks to remind you of medication times, ensuring doses aren’t missed.
Life Expectancy and Living with Lupus
Advancements in treatment have improved life expectancy for those with lupus. With proper management, many can expect to live a normal lifespan. Studies indicate that over 90% of individuals with lupus survive beyond 10 years after diagnosis.
Factors Influencing Life Expectancy
- Organ Involvement: Severe organ involvement, like kidney or central nervous system issues, can affect prognosis, emphasizing the need for timely treatment.
- Infections: Immune-suppressing medications increase infection risk, which remains a leading cause of death in lupus patients. Early prevention and treatment are crucial.
- Cardiovascular Risk: Lupus heightens the risk of heart disease due to chronic inflammation and steroid side effects. Regular monitoring and preventive measures are vital.
- Socioeconomic Factors: Access to healthcare, medication adherence, and lifestyle can significantly influence disease outcomes, highlighting the importance of comprehensive care and support systems.
Enhancing Quality of Life
- Support Network: Building a community through support groups can provide emotional support and practical advice.
- Education: Staying informed about new research and treatment options aids self-advocacy and proactive health management.
- Mental Health Care: Professional counseling can help cope with the emotional challenges of living with a chronic condition.
- Adaptive Strategies: Learning to adapt daily activities, using assistive devices for mobility issues, or adjusting work environments can improve functionality and reduce stress.
Living with lupus requires a comprehensive approach that combines medical management with lifestyle modifications. By understanding symptoms, treatment options, and the importance of ongoing care, individuals with lupus can lead fulfilling lives. Through collaboration with healthcare providers and leveraging support networks, those affected by lupus can navigate the challenges of this chronic disease while maintaining a focus on their overall well-being.