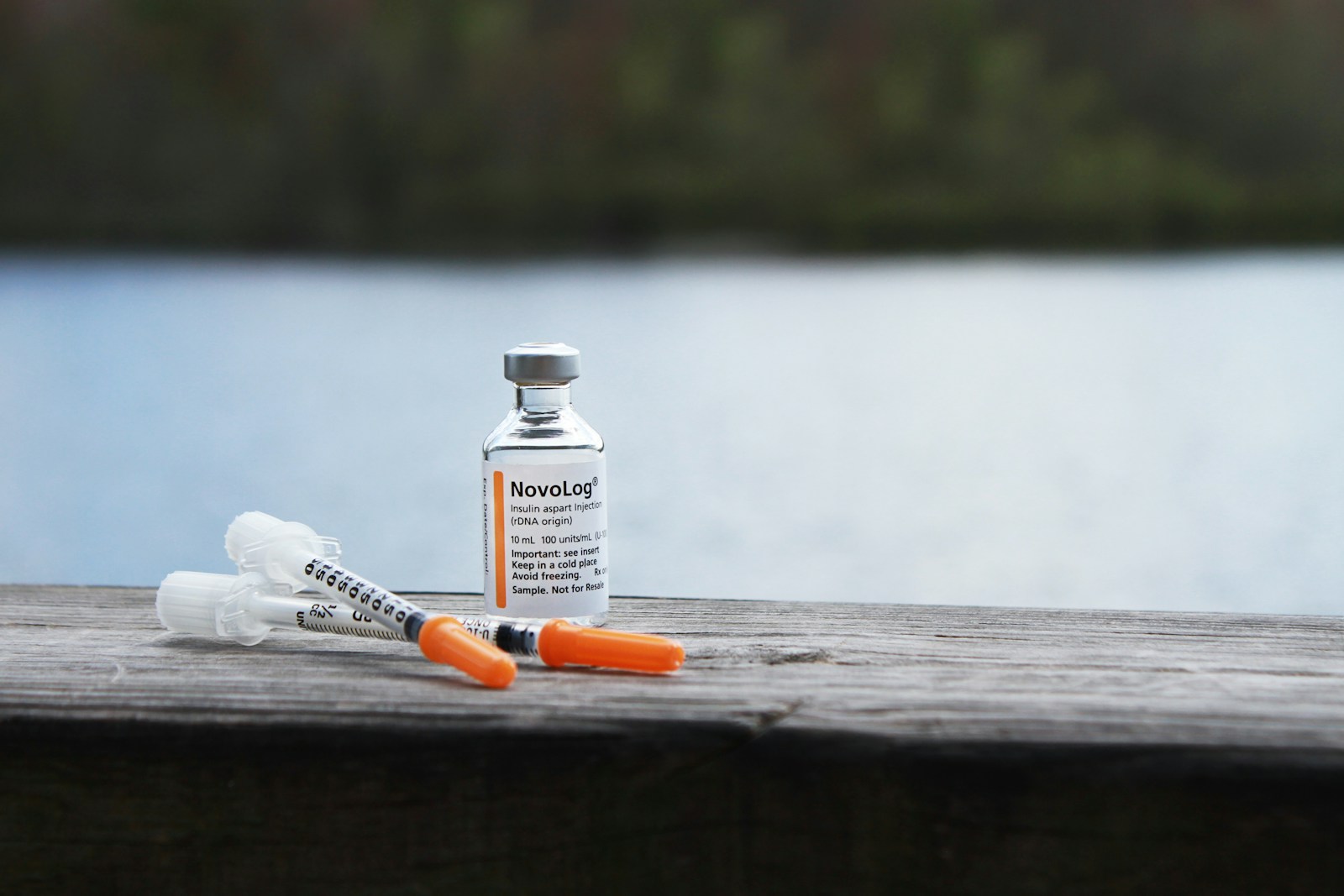
Insulin is a hormone produced by the pancreas, specifically by the beta cells in the islets of Langerhans. It plays a critical role in regulating glucose levels in the blood by facilitating the uptake of glucose into cells, where it is used for energy or stored for later use. Insulin is essential not only for maintaining stable blood sugar levels but also for managing the body’s metabolism of carbohydrates, fats, and proteins. Disruptions in insulin production or function can lead to various metabolic disorders, most notably diabetes.
The Role of Insulin in Glucose Metabolism
The primary function of insulin is to regulate blood glucose levels by promoting the absorption of glucose by cells in the liver, muscles, and fat tissues. When you eat, especially carbohydrate-rich foods, they are broken down into glucose, which enters the bloodstream. As blood glucose levels rise, the pancreas is stimulated to release insulin. Insulin acts like a key, unlocking cells and allowing glucose to enter and be used for energy.
Insulin’s Mechanism of Action
Insulin binds to insulin receptors on the surface of cells, triggering a cascade of events inside the cell. The binding of insulin activates the insulin receptor, which in turn signals other proteins and enzymes within the cell to move glucose transporter proteins (such as GLUT4) to the cell membrane. Once at the membrane, these transporters facilitate the entry of glucose from the blood into the cell.
Key Functions of Insulin Beyond Glucose Uptake
While insulin’s most well-known function is regulating blood sugar, it also has several other vital roles:
- Glycogen Storage: Insulin signals the liver to convert excess glucose into glycogen, which is stored for later use. When blood glucose levels drop, glycogen can be converted back into glucose to maintain stable energy levels.
- Fat Storage and Metabolism: Insulin inhibits the breakdown of fat (lipolysis) in adipose tissue by decreasing the activity of hormone-sensitive lipase, the enzyme responsible for breaking down stored fat into fatty acids. By promoting fat storage, insulin ensures that the body uses glucose as its primary energy source rather than fat.
- Protein Synthesis: Insulin plays a role in protein metabolism by stimulating amino acid uptake and protein synthesis in muscle cells, aiding in muscle growth and repair.
- Inhibition of Gluconeogenesis and Glycogenolysis: Insulin inhibits the liver’s production of new glucose from non-carbohydrate sources (gluconeogenesis) and the breakdown of glycogen into glucose (glycogenolysis), preventing unnecessary increases in blood glucose levels.
Insulin and Diabetes: A Detailed Overview
Diabetes is a chronic condition characterized by problems with insulin production or function. There are two main types of diabetes: Type 1 and Type 2, each with distinct mechanisms and causes.
Type 1 Diabetes: An Autoimmune Disorder
Type 1 diabetes is an autoimmune condition in which the body’s immune system mistakenly attacks and destroys the beta cells in the pancreas that produce insulin. As a result, little or no insulin is produced, leading to chronically high blood glucose levels (hyperglycemia). Without insulin, glucose cannot enter the cells, leaving them deprived of energy while glucose accumulates in the bloodstream.
People with Type 1 diabetes must rely on insulin therapy (injections or pumps) to regulate their blood sugar. Managing Type 1 diabetes requires careful monitoring of blood glucose levels, adjusting insulin doses based on food intake, physical activity, and other factors.
Type 2 Diabetes: Insulin Resistance and Insufficient Production
In Type 2 diabetes, the body’s cells become resistant to the effects of insulin. This resistance means that even though insulin is present, it doesn’t work effectively to lower blood glucose levels. Initially, the pancreas compensates by producing more insulin, but over time, it cannot keep up with the demand, leading to hyperglycemia.
Type 2 diabetes is often associated with obesity, physical inactivity, and a diet high in refined carbohydrates. While it can be managed with lifestyle changes, such as diet and exercise, some people may require medication or insulin therapy as the condition progresses.
Insulin Resistance: The Early Stage of Type 2 Diabetes
Insulin resistance is a precursor to Type 2 diabetes and is characterized by the body’s inability to respond properly to insulin. When cells become resistant to insulin, the pancreas compensates by producing more insulin to try to maintain normal blood glucose levels. Over time, this increased demand on the pancreas can lead to beta cell dysfunction, reducing insulin production and setting the stage for Type 2 diabetes.
Insulin resistance is closely linked to metabolic syndrome, a cluster of conditions including high blood pressure, elevated blood sugar, abnormal cholesterol levels, and excess body fat around the waist. Together, these conditions increase the risk of heart disease, stroke, and Type 2 diabetes.
Types of Insulin Used in Medical Treatment
For individuals who need insulin therapy, there are several types of insulin available, categorized by their onset of action, peak time, and duration:
- Rapid-Acting Insulin: Begins working within 10-15 minutes and peaks in 1-2 hours. It’s commonly used before meals to control postprandial blood glucose spikes. Examples include insulin lispro (Humalog) and insulin aspart (NovoLog).
- Short-Acting Insulin: Takes effect within 30 minutes and peaks in 2-4 hours. It is often used to control blood sugar during meals. Regular insulin (Humulin R, Novolin R) is a common type.
- Intermediate-Acting Insulin: Begins working within 1-2 hours and peaks in 4-12 hours, providing coverage for about half a day. NPH insulin (Humulin N, Novolin N) is an example.
- Long-Acting Insulin: Provides a steady release of insulin over 24 hours, mimicking the body’s basal insulin secretion. It’s typically taken once or twice daily. Examples include insulin glargine (Lantus) and insulin detemir (Levemir).
- Ultra-Long-Acting Insulin: Lasts more than 24 hours and is taken once daily. Insulin degludec (Tresiba) is a common example, offering flexibility with dosing time.
Combination insulin therapies are also available, mixing different types of insulin to provide both immediate and long-lasting blood sugar control.
Insulin’s Role in Other Metabolic Conditions
Beyond diabetes, insulin is involved in other metabolic conditions. For example, hyperinsulinemia (excess insulin in the blood) is often seen in insulin resistance and is linked to obesity, polycystic ovary syndrome (PCOS), and cardiovascular disease. Elevated insulin levels can drive fat storage and contribute to weight gain, leading to a cycle of worsening insulin resistance.
Conversely, insulin deficiency, whether due to autoimmune destruction in Type 1 diabetes or pancreatic exhaustion in advanced Type 2 diabetes, can lead to diabetic ketoacidosis (DKA), a serious and potentially life-threatening condition. DKA occurs when the body breaks down fat at an accelerated rate, leading to the accumulation of ketones, which make the blood acidic.
Insulin and the Future of Treatment
Research into insulin therapies continues to advance, with developments like smart insulin pens, continuous glucose monitors (CGMs), and insulin pumps that automatically adjust dosing based on real-time blood glucose readings. These technologies aim to improve glycemic control, reduce the risk of complications, and enhance the quality of life for people with diabetes.
In addition, scientists are exploring potential treatments like stem cell therapy and pancreatic islet cell transplants, which could provide more permanent solutions for those who need insulin. The development of artificial pancreases, combining insulin pumps and CGMs, represents a significant step forward in mimicking the body’s natural insulin production.
The Crucial Role of Insulin
Insulin is far more than just a hormone for managing blood sugar; it’s central to how your body processes energy, stores nutrients, and maintains metabolic balance. Disruptions in insulin production or function can lead to serious health conditions like diabetes, metabolic syndrome, and other disorders. Whether your body produces insulin naturally or you rely on external insulin therapy, understanding how insulin works is essential for maintaining health and managing metabolic diseases effectively.
As research and technology continue to evolve, the future of insulin therapy and diabetes management promises even greater advancements, offering hope for better control and potentially curative treatments. Insulin remains one of the most critical components of metabolic health, making its role in both everyday life and medical science indispensable.